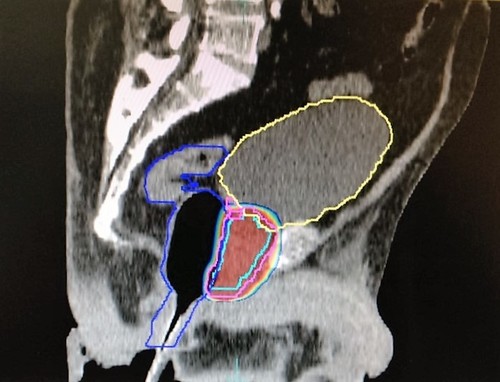
Prostate Caddy™ can help minimize prostate movement during treatment. The use of these devices is associated with reduced prostate motion and stabilized prostate displacement during the treatment course (4).
Prostate Caddy™ supports reproducible results when used with a consistent fill volume and insertion depth over the treatment course. Daily rectal balloon use reduces prostate movement in between treatments, maintains anterior rectal wall position, and supports a reduced rectal margin through proper immobilization (2).
Prostate Caddy™, when properly positioned and inflated, separates the posterior rectal mucosa. Rectal balloon use reduces the rectal wall volume exposed to doses greater than 40 Gy (1)(3)(7) and associated late toxicity.
Hypofractionated treatments and dose escalation benefit from the use of rectal balloons (5)(7).
Historically, larger and wider rectal balloons are associated with discomfort and poor compliance (6). The smaller design of Prostate Caddy™ keeps discomfort to a minimum.
Traditional rounded balloon designs push the anterior rectal mucosa against the prostate and compress the prostate/rectum interface. Prostate Caddy™ has a patented longitudinally symmetric barrel-shaped design that reduces anatomical distortion of the prostate interface.
Rounded atraumatic tip and improved room temperature stiffness facilitate insertion. The thermo-sensitive polymer of the central lumen maximizes comfort and conforms to the patient’s anatomy.
Prostate Caddy™ has depth markings along the central lumen and a 2-way locking stopper to secure the insertion depth of the balloon for day-to-day consistency. This device also comes equipped with a reliable inflation/deflation valve with luer lock connection to facilitate reproducible inflation volume.